As mentioned by @Angel_Myers, CGMs from Abbott and Dexcom can be inaccurate in the lower range of 80-120 mg/dL. You can use a conventional blood glucose monitor to confirm this.
Additionally, I recommend looking into lithium supplementation.
5 Likes
There is a study that finds that — in fruit flies.
2 Likes
Which is why I think we need a bit more of a focus on multiple N=1 biohacking.
2 Likes
Beth
#60
John, are you saying that after 140 is when I should worry? I wasn’t sure what 8/140 meant (the ‘8’)
I guess I need to consider taking a higher dose of metformin or perhaps consider adding acarbose that seems to be very popular here.
1 Like
I was confused at first too, but I think 8 is in different units. 140 would be mg/dL. 8 would be mmol/L.
1 Like
Last week’s 3mg was uneventful. I took it friday night before sleeping so I’d be in a fasted state before and after the dose.
This friday, I forgot and took it saturday afternoon after lunch. I waited until my BG was stable ~3 hours after the meal and took 4mg. After about 45 minutes I noticed my BG rose about 25 mg/dL and I had to exercise it off. When I sat back down it went up slightly again before stabilizing.
I think this is more evidence that taking rapamycin immediately shuts down or lowers insulin production in me and I should avoid taking it while not fasted.
First week, took 2mg 30 min after a meal → big spike
Third week, took 3mg in a fasted state and didn’t eat for 8 hours after dosage → no spikes while I slept
Fourth week, took 4mg 3 hours after a meal → small spike
4 Likes
The strict conversion is 8 mmol/L or 144 mg/dL, but people tend to think of thresholds of 10 mg/dL.
Ideally, however, your body would keep glucose levels below the point at which I think the inositol pathway gets engaged. A quick google search did not find a good reference for this. If people want one I will put some time in. I probably recorded the reference when I found this useful bit of information.
2 Likes
Neo
#64
Yes, that would be very valuable John!
This comes from starting with the Polyol pathway and Chris MasterJohn has written about this here:
When blood glucose rises above 140 mg/dL, this is the approximate point at which it spills into the polyol pathway at a greater-than-normal rate, which represents a suboptimal state of metabolism that is likely to hurt antioxidant status and compromise detoxification pathways as well as the recycling of vitamin K and folate. It must be kept in mind that a healthy person will adapt to glycemic loads they consume regularly. Thus, a one-time spike above 140 mg/dL should never be used to conclude anything whatsoever. Only repeated spikes above this level with repeated consumption of the same glycemic load over several days to several weeks should be used as a cause for concern.
This may be better as well
3 Likes
Glucose will increase with stress, and rapamycin seems to simulate stress in the body. I wonder if the increase is similar to the increase you see with stress. When diabetics are stressed, it is difficult to control their glucose. Any non-diabetics out there using a continuous glucose monitor and taking rapamycin?
1 Like
Beth
#67
That would be me. I’ve had a couple conversations with my doc this week because my cgm is showing my rapa is causing very abnormal spiking… I’m prone to it anyway and take metformin, but it’s nuts since rapa (it’s what it was before starting metformin)
1 Like
Beth
#68
This is very helpful, thank you!
After texting my doc my cgm data showing my spike going over 200, we just talked and he suggested instead of taking metformin twice during the day that I experiment with taking it before bed. I didn’t understand why but he explained when taken before bed, it can help affect cortisol in the morning. Doing that might help me self regulate all day. I don’t really understand it nor do I need to, but I’ll give it a shot. If this doesn’t work, we will then see how I tolerate acarbose (he said gi effects are likely). Thoughts?
1 Like
Are your spikes only with meals? Do you take rapamycin once per week, and if so, are your glucose levels more difficult to control for the days immediately following taking rapamycin? How high are your spikes, and do they correlate with high-carbohydrate meals? Do you know your HbA1c?
1 Like
If Metformin is often added to Rapamycin to control blood sugars and Rapamycin is taken once per week, is anyone pulsing Metformin? I think pulsing Metformin would decrease the problems with exercise but still give control while the Rapamycin serum levels are elevated (assuming the elevation is from the Rapamycin). Do most non-diabetics see problematic elevations in their blood sugars with continuous glucose monitors while taking Rapamycin? I am assuming problematic would be peaks above 180 or 200.
In Matt Kaeberlein’s latest video he says on the first couple days days following his dose, his blood glucose does a “jumpy” pattern which matches mine and other peoples’ experience here. He also said by the 3rd day it settles down again which matches my timeline exactly.
6 Likes
Beth
#72
Karl, I’ll check my data and will come back here for an update.
PBJ
#73
I still do not see any reason not to fast or use a fasting mimicking diet on the day/days after rapa administration. If I can keep my glucose in better control without added medications, that seems like a logical approach. Some people are scared to lose a day of growth when that is the ultimate goal anyhow.
Yes, I’ve seen a number of people note in past discussions that they take metformin only on the day they take rapamycin, for this reason.
Fifth week, took 4mg in a fasted state before bed → no spikes while I slept. Completely stable at a healthy low-mid 90s.
Skipped breakfast and lunch the following day and had a $5 Mcdonald’s meal for dinner. Diet coke + McDouble + small fries + nuggets. I chose this meal as a worst case bad diet scenario glycemic load test and was pleasantly surprised to see the spike peak at only 159 mg/dl before coming back down to 108 with exercise. After exercise, it went back up to the 120s but fluctuated in a jigsaw pattern like I’ve seen before in the first 3 days of dosing and others have reported, before settling back down.

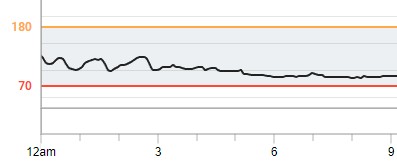
3 Likes
Had my bloodwork done this week.
Unfortunately the often report lipid effects seem to affect me too. Numbers are ~2 months apart. I also did a 2 week washout where I stopped my weekly rapa dose.
Total cholesterol: 212 → 244
Triglycerides: 104 → 127
HDL: 61 → 64
VLDL: 18 → 22
LDL: 133 → 158
LDL/HDL ratio: 2.2 → 2.5
ApoB: 113 (test 2 months ago didn’t measure ApoB)
From reading some studies, it seems mTORc1 actively inhibits lipolysis so inhibiting mTORc1 would stimulate your adipocytes to dump its lipid contents into the bloodstream. I’ve also been caloric restricting which would likely do the same.
Physically, I’ve noticed a pretty rapid loss of body fat. I can see my ribs with my shirt off, which was not the case prior to starting rapamycin 2 months ago. I’ve also put on more lean mass from increased exercising (due in part to wanting to counter rapa’s glucose effects).
On that note, my glucose levels have all improved drastically from my pre-rapa days.
Fasting levels: 99 (january) → 93 (late May) → 83 (this week)
hba1c: 5.5% → 5.6% → 5.3%
2 Likes