I suspect we will find separate additive benefit from GLP that gets into the brain having GLP activity in the brain, which is different from the functional changes seen powerfully through signaling from the vagus nerve, which the newer agents are more potent for.
I’m favoring a dulaglutide and tirzep or retatrutide blend to hit GLP through both ways.
I have access to this compounded upcoming on the dulaglutide and the others.
1 Like
adssx
#338
Association analyses of nutritional markers with Parkinson’s disease and Alzheimer’s disease
Apolipoprotein B, low-density lipoprotein, and total cholesterol reduce PD risk, while homocysteine increase PD risk.
Apolipoprotein A1 is a protective factor for AD, while homocysteine is a risk factor for AD.
Based on other MR studies, ApoB, LDL and TC are probably causal for PD, while Hcy is not.
This recent paper (Identifying potential causal effects of Parkinson’s disease: A polygenic risk score-based phenome-wide association and mendelian randomization study in UK Biobank) also identified as risk factors for PD: “fluid intelligence score” and “average total household income before tax” and as protective factors “maternal smoking around birth, playing computer games, salt added to food, and time spent watching television”
So PD is really the disease of healthy people: smoking, dyslipidemia, diabetes, obesity, poor diet, and television are protective while intelligence and high income are risk factors 
3 Likes
Pender
#339
Nilotinib improved biomarkers and cognitive outcomes for Lewy body in a phase 2 trial.
It’s a relatively small study (43 adults), so didn’t achieve significance on most biomarkers (but did see positive differences).
It did achieve significance on:
- CSF dopamine levels
- Alzheimer’s Disease Assessment Scale-Cognitive Subscale 14 (ADAS-Cog14)
- MDS-UPDRS Part I (cognition)
At a dose of 200 mg once daily, “all the biomarkers and all the clinical and cognitive outcomes were moving in the correct direction,” Turner reported.
Nilotinib was safe and well tolerated, with more adverse events noted in the placebo group (74 vs 37; P = .54). There was an increase in the levodopa equivalent daily dose in the placebo group, but no significant increase or no change in the nilotinib group, which would suggest more parkinsonism or disease progression in the placebo group.
Notably, Turner added, there were fewer falls in the nilotinib group than the placebo group (6 vs 21) — a “70% reduction,” which could be due to improved cognition with nilotinib.
Source: https://www.medscape.com/viewarticle/leukemia-drug-shows-promise-lewy-body-dementia-2024a1000k73?form=fpf
1 Like
adssx
#340
This is amazing. Has there ever been a successful phase 2 trial for LBD? It might be a first! Can’t wait for the phase 3! How safe is nilotinib? Can it be used for “longevity” / “neuroprotection” purposes @DrFraser? I’ll sponsor nilotinib in C. Elegans and see…
1 Like
adssx
#341
Not so fast for nilotinib in PD: RENEWAL: REpurposing study to find NEW compounds with Activity for Lewy body dementia—an international Delphi consensus 2022
In clinical studies, the use of nilotinib in PD has so far yielded inconclusive results. A trial in 75 patients with PD randomised to receive placebo, nilotinib 150mg or 300mg for 12 months showed that nilotinib is safe, well tolerated and can increase dopamine metabolites in the CSF as well as reduce CSF α-synuclein oligomers and hyperphosphorylated tau [50]. An open-label extension of this study that included 63 patients for an additional 12 months randomised to receive 150mg or 300mg nilotinib showed that nilotinib continued to be safe and tolerated and demonstrated that nilotinib 300mg was associated with stable scores in the Movement Disorder Society Unified Parkinson’s Disease Rating Scale (MDS-UPDRS) from baseline to 27 months in parts I (nonmotor including cognitive) and II (activities of daily living), while nilotinib 150mg was associated with improvement in the sum of UPDRS Part I (nonmotor including cognitive) and II (activities of daily living) with no difference in the UPDRS Part III (motor examination) [51]. Quality of life measures also worsened in the nilotinib 150mg compared to 300mg group between 15 and 27 months [51]. However, another double-blind placebo-controlled study that enrolled 76 patients with PD who received nilotinib 150mg or 300mg or placebo for 6 months showed that, while nilotinib was safe and well tolerated, patients in the nilotinib arms showed worse motor scores (measured with the MDS-UPDRS) [52]. This study failed to identify any changes in the dopamine metabolites in the CSF and suggested that, at least for PD, there was no evidence to support further testing of nilotinib.
Other ongoing trials of drugs from the same family (or related):
I’ve just sponsored nilotinib and bosutinib in the MMC. Dasatinib previously failed (could be a dose issue though?):
3 Likes
adssx
#342
Accelerating assessment of disease modification in Parkinson’s via multi-arm, multi-stage design: the EJS ACT-PD initiative 2024
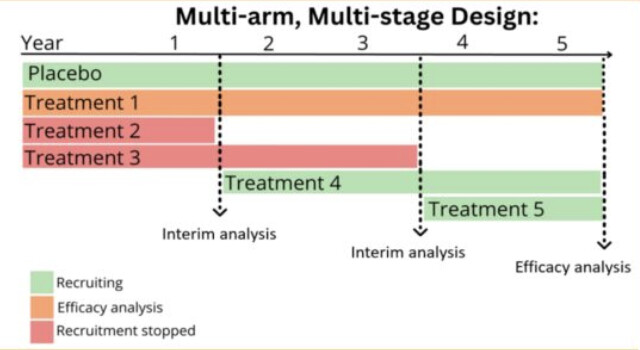
They’re starting a multi-arm, multi-stage (MAMS) trial platform in the UK to accelerate research: one shared placebo arm to lower cost and lower the % of participants with placebo (to increase the willingness to join the trial) + continuous assessment and if one treatment doesn’t work it’s directly replaced by the next candidate in a ranked list of compounds:
Ranking process:
The top candidates that will move to trial are:
- Telmisartan 40 mg
- Terazosin 5 mg
- Ursodeoxycholic acid (UDCA, ursodiol) 2.5 g
(source)
Ideally the industry will join the trial at some point and the platform will be self-funded with many more arms.
2 Likes
A_User
#343
Did you mean 250 mg? The dosing for gallstone prophylaxis is 600 mg a day, and dissolution is 8 - 10 mg/kg/day.
I’ve been looking into TUDCA which is the same but taurine attached, and OTC, because I think I have gallstones and I would guess it’s good to try and dissolve them (because my ALP is high - higher ALP associated with higher ACM). 1 in 7 have asymptomatic gallstones.
1 Like
adssx
#344
Oops sorry edited: 2.5 g. So quite high indeed.
2 Likes
I have small, asymptomatic gallstones, diagnosed with US imaging. What do you consider high ALP? Mine has been steadily climbing through the years, and now stands at 73 U/L (range at UCLA labs: 37 - 113 U/L), tested a couple of weeks ago (age 66).
A_User
#346
Optimal value based on association studies is 50 U/L:
2 Likes
Thanks, AnUser. I guess I have to find a way to lower my ALP.
adssx
#348
Serum 25-hydroxyvitamin D concentrations and their impact on all-cause mortality in Parkinson’s disease: insights from National Health and Nutrition Examination Survey 1999–2020 data 2024
The analysis showed a U-shaped curve between 25(OH)D levels and mortality risk, with the lowest risk at 78.68 nmol/L (p-non-linear = 0.007, p-overall = 0.008). Kaplan–Meier analysis found the highest survival rates in patients with 25(OH)D levels between 75–100 nmol/L (p = 0.039). Compared to this group, patients with levels below 50 nmol/L had a 3.52-fold increased mortality risk (95% CI = 1.58–7.86, p = 0.002), and those above 100 nmol/L had a 2.92-fold increase (95% CI = 1.06–8.05, p = 0.038). Age-specific subgroup analysis (p = 0.009) revealed that both very low (<50 nmol/L) and high (>100 nmol/L) levels increased mortality risk in patients under 65, while levels below 75 nmol/L raised mortality risk in older patients.
3 Likes
adssx
#349
Maybe I’m missing something here, but genetic factors that predict a high Vitamin D level … do we have actual data on subjects on what their level was? I could have genetic factors that favor a higher level, but get no sun and consume no vitamin D. I could have genetic factors that predict low, but I supplement.
I’m much more interested in actual serum levels over the long term and outcomes.
I’d like to know how this properly gets controlled for as it isn’t quite the same thing as saying no relationship between vitamin D levels and PD.
1 Like
adssx
#351
You’re right but here we have both the MR and the long-term association study showing that vitamin D is not essential in PD: you just don’t want to be below 75 nmol/L. Parkinson’s patients supplementing with vitamin D also don’t do better than non-users: Parkinson Symptom Severity and Use of Nutraceuticals (whereas those supplementing with glutathione, lithium, curcumin, omega 3 or vitamin B12 do for instance). So it’s good to be able to focus on what moves the needle most.
1 Like
Yes, that is a fair call, but I’d still measure and treat low Vitamin D, but not necessarily for PD, but probably for AD.
Luckily I regularly advise all the items that are protective for PD as they also seem to be items protective for AD and vascular disease to some extent.
It actually takes some work for most people to be at 75 nmoL/L as I think the normal is typically 30-100, and so many of my patients before supplementation, including many who have lots of time outside end up being in the high 20’s through low 40’s. So worth measuring.
1 Like
adssx
#353
You’re right that vitamin D seems protective in AD and people with PD are at high risk of AD:
50 nmol/L = 20 ng/mL only!
I know you like people to be 50–70 ng/mL (125–175 nmol/L) but it seems that for both AD and PD the optimal is 75–100 nmol/L (30–40 ng/mL).
2 Likes
I’d be happy to get 40 ng/ml! I’m struggling to get 30 even with 10,000 IUs supplementation.
75 ng/ml seems impossible.
It takes 3-6 months of dosing to get a steady state as is fat soluble. I’d recommend you read the Target D Trial as that will give some context. But I’d stick with 10,000 IU/day, test at 3 month intervals and it will likely climb up nicely over time. There are a segment of the population that seems to require more than 10,000 IU. Also with Vitamin D, make sure to take it with Vitamin K2 (I prefer MK7 over MK4) of at least 200 mcg/day.
It’s my best assessment right now, that 10,000 IU/day will get people to 50-70 almost always, but it might take 6-12 months, and as that point if not optimal, then go up in dose, but that would be really rare.
1 Like