adssx
#342
Accelerating assessment of disease modification in Parkinson’s via multi-arm, multi-stage design: the EJS ACT-PD initiative 2024
They’re starting a multi-arm, multi-stage (MAMS) trial platform in the UK to accelerate research: one shared placebo arm to lower cost and lower the % of participants with placebo (to increase the willingness to join the trial) + continuous assessment and if one treatment doesn’t work it’s directly replaced by the next candidate in a ranked list of compounds:
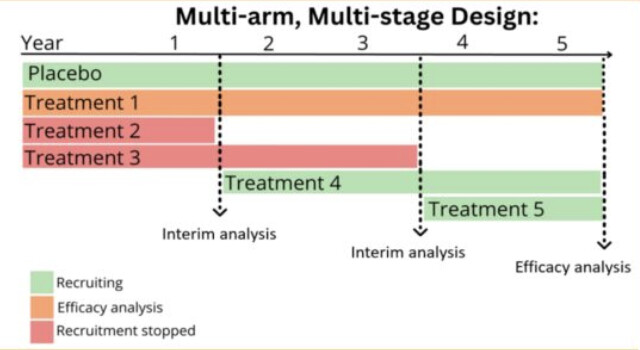
Ranking process:
The top candidates that will move to trial are:
- Telmisartan 40 mg
- Terazosin 5 mg
- Ursodeoxycholic acid (UDCA, ursodiol) 2.5 g
(source)
Ideally the industry will join the trial at some point and the platform will be self-funded with many more arms.
2 Likes
A_User
#343
Did you mean 250 mg? The dosing for gallstone prophylaxis is 600 mg a day, and dissolution is 8 - 10 mg/kg/day.
I’ve been looking into TUDCA which is the same but taurine attached, and OTC, because I think I have gallstones and I would guess it’s good to try and dissolve them (because my ALP is high - higher ALP associated with higher ACM). 1 in 7 have asymptomatic gallstones.
1 Like
adssx
#344
Oops sorry edited: 2.5 g. So quite high indeed.
2 Likes
I have small, asymptomatic gallstones, diagnosed with US imaging. What do you consider high ALP? Mine has been steadily climbing through the years, and now stands at 73 U/L (range at UCLA labs: 37 - 113 U/L), tested a couple of weeks ago (age 66).
A_User
#346
Optimal value based on association studies is 50 U/L:
2 Likes
Thanks, AnUser. I guess I have to find a way to lower my ALP.
adssx
#348
Serum 25-hydroxyvitamin D concentrations and their impact on all-cause mortality in Parkinson’s disease: insights from National Health and Nutrition Examination Survey 1999–2020 data 2024
The analysis showed a U-shaped curve between 25(OH)D levels and mortality risk, with the lowest risk at 78.68 nmol/L (p-non-linear = 0.007, p-overall = 0.008). Kaplan–Meier analysis found the highest survival rates in patients with 25(OH)D levels between 75–100 nmol/L (p = 0.039). Compared to this group, patients with levels below 50 nmol/L had a 3.52-fold increased mortality risk (95% CI = 1.58–7.86, p = 0.002), and those above 100 nmol/L had a 2.92-fold increase (95% CI = 1.06–8.05, p = 0.038). Age-specific subgroup analysis (p = 0.009) revealed that both very low (<50 nmol/L) and high (>100 nmol/L) levels increased mortality risk in patients under 65, while levels below 75 nmol/L raised mortality risk in older patients.
3 Likes
adssx
#349
Maybe I’m missing something here, but genetic factors that predict a high Vitamin D level … do we have actual data on subjects on what their level was? I could have genetic factors that favor a higher level, but get no sun and consume no vitamin D. I could have genetic factors that predict low, but I supplement.
I’m much more interested in actual serum levels over the long term and outcomes.
I’d like to know how this properly gets controlled for as it isn’t quite the same thing as saying no relationship between vitamin D levels and PD.
1 Like
adssx
#351
You’re right but here we have both the MR and the long-term association study showing that vitamin D is not essential in PD: you just don’t want to be below 75 nmol/L. Parkinson’s patients supplementing with vitamin D also don’t do better than non-users: Parkinson Symptom Severity and Use of Nutraceuticals (whereas those supplementing with glutathione, lithium, curcumin, omega 3 or vitamin B12 do for instance). So it’s good to be able to focus on what moves the needle most.
1 Like
Yes, that is a fair call, but I’d still measure and treat low Vitamin D, but not necessarily for PD, but probably for AD.
Luckily I regularly advise all the items that are protective for PD as they also seem to be items protective for AD and vascular disease to some extent.
It actually takes some work for most people to be at 75 nmoL/L as I think the normal is typically 30-100, and so many of my patients before supplementation, including many who have lots of time outside end up being in the high 20’s through low 40’s. So worth measuring.
1 Like
adssx
#353
You’re right that vitamin D seems protective in AD and people with PD are at high risk of AD:
50 nmol/L = 20 ng/mL only!
I know you like people to be 50–70 ng/mL (125–175 nmol/L) but it seems that for both AD and PD the optimal is 75–100 nmol/L (30–40 ng/mL).
2 Likes
I’d be happy to get 40 ng/ml! I’m struggling to get 30 even with 10,000 IUs supplementation.
75 ng/ml seems impossible.
It takes 3-6 months of dosing to get a steady state as is fat soluble. I’d recommend you read the Target D Trial as that will give some context. But I’d stick with 10,000 IU/day, test at 3 month intervals and it will likely climb up nicely over time. There are a segment of the population that seems to require more than 10,000 IU. Also with Vitamin D, make sure to take it with Vitamin K2 (I prefer MK7 over MK4) of at least 200 mcg/day.
It’s my best assessment right now, that 10,000 IU/day will get people to 50-70 almost always, but it might take 6-12 months, and as that point if not optimal, then go up in dose, but that would be really rare.
1 Like
I use dedrogyl (which is 25OHD) to increase the level. I take 3,000 iu a day which does not maintain the level and dedrotyl once a week either to maintain or increase the level. There are probably foods with a high level of 25OHD.
It seems that the body does not metabolise cholecalciferol that well.
1 Like
adssx
#358
Are you sure we’re using the same units? 30 nmol/L is 12 ng/mL. Severe deficiency starts below 5 ng/mL.
1 Like
@adssx Yes, you are correct. My last test was 31 ng/ml. My personal goal is 50 ng/ml.
1 Like
adssx
#360
Then at 31 ng/mL, if the papers above are correct you are PERFECT for AD and PD risk, as the optimal seems to be around 80 nmol/L = 32 ng/mL.
1 Like
Yeah, I did think there must be a unit confusion, but wasn’t sure, good catch. It’s funny, because my latest reading is 38ng, and looking at the literature I really don’t see why I should go higher. It may be the case that depending on what you are trying to address (ACM, PD, bone health etc.), the ideal level will be different. You can’t just pick ACM, because as individuals, we die from our specific weakest link, which will be different for everyone - we are not “population”, we’re n=1. Therefore ACM for a populace or cohort may not be the optimal outcome to look at, instead it should be the outcome for the specific issue you’re trying to address.
1 Like