A_User
#23
If you are lower BMI what do you think about bone health and risk for hip fractures, etc?
2 Likes
Tirzepatide - StatPearls - NCBI BookshelfNcbi.nom.nih.gov/books/NBK585056/
This goes through things pretty nicely - we’d expect increased insulin levels.
@A_User The issue is slow weight loss and making sure adequate exercise. No more than 1 lb/week, and make sure doing weight lifting plus aerobic stuff, and preferably track via DEXA and if not available by impedance scale to make sure no more than 20% or so of weight loss is muscle. If you lose fast, you’ll have a high % as muscle. Same issue with risks for osteoporosis.
3 Likes
Id expect insulin should help prevent muscle loss?
Neo
#26
But perhaps offset some of the CR benefits?
Neo
#27
For someone who already is at optimal and body composition (and not at increased risks of neurodegeneration), do you have a view/any thoughts on the net trade of walking around with higher insulin levels (net negative for longevity) and other longevity benefits of GLP-1A?
Been using TZ since July 2024. Using a 3.5mg weekly dose I’ve lost 50lb’s since then. I’m not diabetic but was getting in the pre-diabetic range. Last annual blood test in Jan indicates that has moved in the right direction as expected.
I have 12 of the 13 top fat genes turned on and am in the non-responder group for weight loss through diet and exercise.
I received a sample of Retatrutide a month ago and tried 4mg and it was impressive. I had plateaued at 153 - 54 lb for a couple months (my ideal wight should be 145) but was quite happy as I have not been below 180 in 25 years.
With RT (2 weeks) I have dropped a bit more, now down to 149 and have found it has really reduced cravings and hunger and increased satiety.
I have a Withings Body Cardio scale and it measures more than just weight. My muscle mass did drop a bit but leveled off after the first 3 months. My BMI is now 24, where it had been 34.
Overall I’m super impressed as are my friends who I’ve been helping with this.
My test results are in this thread.
2 Likes
I do have thoughts on this - insulin is toxic to blood vessels - not nearly as badly as high glucose is. I’m not sure that if you are already ideal body weight, insulin sensitive that I’d be rushing to do this. If at risk of neurodegeneration, use a weak GLP that crosses the blood brain barrier and then the weight loss isn’t and issue, and the bump in insulin is likely not near as relevant - but without risks, I’m not sure I’d be putting a GLP-1 up as a top choice.
2 Likes
I’d probably just opt for an SGLTi like empagliflozin for all the other benefits and you don’t have to worry about overdoing it like on a GLP1. Although it depends on how much weight you need to lose. You can even increase your food intake and lose weight like the folks in this study.
At week 90, weight loss averaged −3.2 ± 4.2 kg (corresponding to a median calorie deficit of 51 kcal/day [interquartile range (IQR) 112]). However, the observed calorie loss through glycosuria (206 kcal/day [IQR 90]) was predicted to result in a weight loss of –11.3 ± 3.1 kg, assuming no compensatory changes in energy intake. Thus, patients lost only 29 ± 41% of the weight loss predicted by their glycosuria; the model indicated that this difference was accounted for by a 13% (IQR 12) increase in calorie intake (269 kcal/day [IQR 258]) coupled with a 2% (IQR 5) increase in daily energy expenditure (due to diet-induced thermogenesis). This increased calorie intake was inversely related to baseline BMI (partial r = −0.34, P < 0.01) and positively to baseline eGFR (partial r = 0.29, P < 0.01).
Chronic glycosuria elicits an adaptive increase in energy intake. Combining SGLT2 inhibition with caloric restriction is expected to be associated with major weight loss.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4542276/
1 Like
I have a question!!
Since insulin is anabolic and supports muscle health, I’ve been wondering if all the claimed muscle loss issues may be measurement issues?
I do notice fluctuations in my “measured” muscle mass depending on if I’m gaining weight or losing weight VS a stable weight.
Could inter-muscular fat be skewing what people perceive as muscle loss?
When I’m gaining weight, usually fat  my measured muscle mass goes up.
my measured muscle mass goes up.
When I’m losing fat my measured muscle mass goes down, until I stabilize the weight and then it comes back up a bit. Generally not back to my “fat boy” levels. And that is what makes me question this idea of muscle loss when using GLP1-R peptides.
I also measure bicep circumference and as expected, it goes down when I’m losing fat but my muscle tone stays excellent and my strength is not an issue.
So I’ve been confused by all the naysayers on the muscle loss thing. Maybe because I measure every day and have data that most of the naysayers don’t have in their process?
1 Like
Steve,
Sorry for the delay - it’s been a busy day of consults. This is a really good question. Intramuscular fat causes insulin resistance and stops muscle from uptaking glucose. So it’s a bad thing, and great to get rid of. I’m not sure that our impedance testing really lets us know this, and I doubt most of us going running out for a DEXA each time we get a bit fat or thin.
Muscle with a lot of fat doesn’t really function well, so I doubt this is what is going on. Generally rapid weight loss favors taking significant muscle as part of it, and then when gain weight just do it as fat resulting in overall loss of good body architecture.
I have people make sure no more than 1 lb/week, and make sure doing weight lifting in addition to weight bearing exercise during this to mitigate muscle loss.
I would simply guess that you are using impedance testing if doing it every day, and the devices typically use a lot of calculations and assumptions that may not actually be applicable or accurate in this setting.
Bottom line … I don’t know, but these are my thoughts on this.
3 Likes
Yes the scale I use does impedance measurements. The Withings Body Cardio scale.
It’s been determined that it is quite accurate for PWV. But I agree that it is not as accurate for overall body composition but this study does indicate the body mass measurement is probably accurate enough outside clinical study requirements. So I take the data as a “trend” type. To see trends as opposed to absolute values.
Withings Body Cardio Versus Gold Standards of Pulse-Wave Velocity and Body Composition
Conclusions: The Body Cardio scale provides accurate measures of BM and PWV; however, it should be used cautiously for measures of FM and FFM.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7151625/
2 Likes
I don’t not have even mild metabolic dysfunction but I can say this is also the best medication I’ve ever used. I have lupus and the effect on inflammation is incredible.
4 Likes
A_User
#36
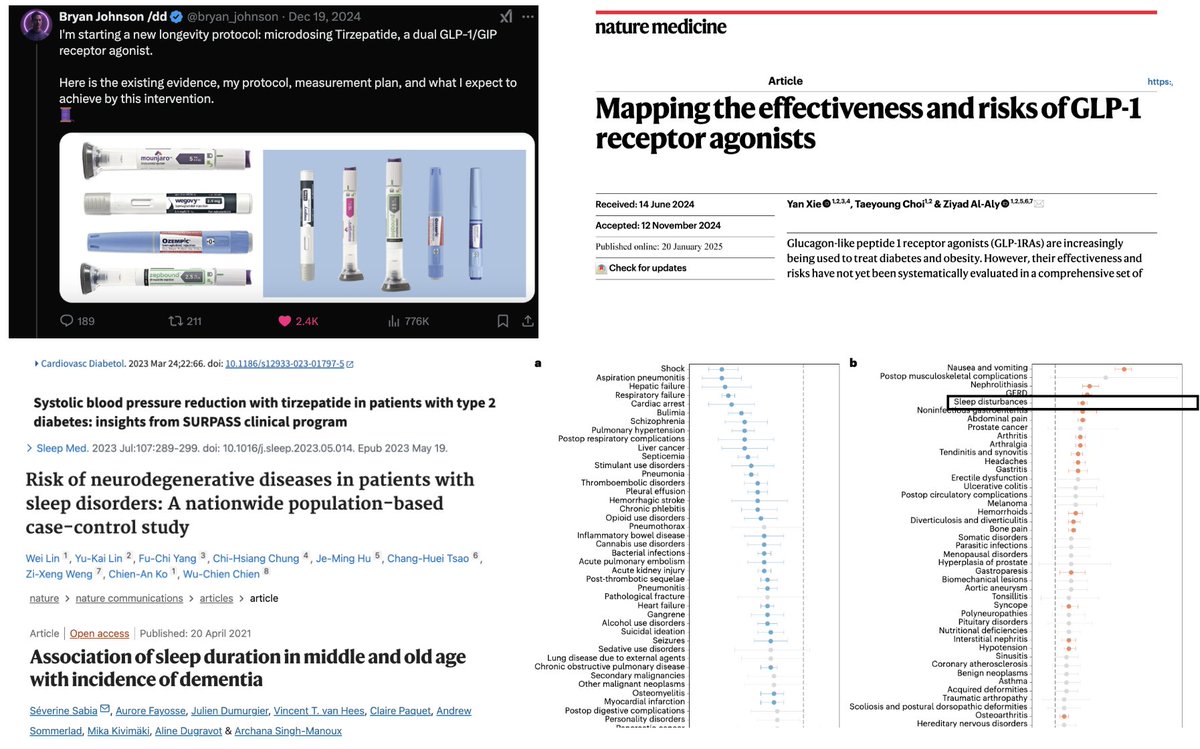
Bryan Johnson quits Tirzepatide:
I am halting Tirzepatide microdosing because it increased my resting heart rate by 3 bpm, lowered my HRV by 7 and decreased my sleep quality by 10%
After 3 weeks of microdosing Tirzepatide, I decided to stop the intervention, here is why:
My resting heart rate (RHR) increased by 3 bpm, a relatively large increase of 7% considering my RHR of mid 40s bpm. A review of 5 clinical trials with 4199 total participants found that, despite lowering blood pressure, the lowest dose (5 mg/week) of Tirzepatide increased HR by 1-4 bpm, interesting to see my microdose at 0.5 mg/week showing similar side effects.
A lower RHR is foundational to perfect sleep. The increase in my RHR decreased my HRV by 7 points, and decreased sleep quality by 10%.
In light of this we had to reevaluate the risk/benefit balance of this intervention:
Benefits: immediate benefits are mostly linked to metabolic optimization (I am already metabolically optimized), newer results support metabolic/obesity independent longevity effects especially for reducing dementia risk, but these are very long term with no readily measurable effect.
Risks/harms: I measured a 7% increase in RHR leading to an average of ~10% drop in sleep quality.
Verdict: the risk/harm outweighs the benefit, for the following reasons
-
Only the non-metabolic longevity benefits are applicable in my case, these were very recently identified, with only a handful of studies supporting them.
-
Even if the longevity benefits (e.g. reduced dementia risk with Tirzepatide) the damage from the long-term reduction in sleep quality is way more likely to outweigh the benefit, than vice versa.
-
For example: a very recent meta-analysis found that diabetics on GLP1-RAs had a 5% reduced risk of neurodegenerative diseases (12% risk reduction for Alzheimer disease), interestingly the same analysis found patients on GLP1-RAs to be at 12% increased risk of developing sleep disturbances. Here we must factor in that having a sleep disorder even for less than 1 year was associated with a 63.8% increase in the odds of developing a neurodegenerative disease, and persistent shorter sleep (6 hours or shorter) in 50s and 60s was associated with a 30% increase in dementia risk by 30%.
-
The former example makes it clear why any potential longevity benefits (mostly applicable to metabolically sick people, including diabetics, and still in need of further data to better confirm and understood), is not worth risking my sleep quality, especially with only 3 weeks on a microdose being enough to start dislodging my perfect sleep.
Caveat: This does not apply to everyone. It should be clear that my risk/benefit profile does not apply to most people in need of metabolic optimization or weight-loss, for these the benefits of GLP1-RAs probably outweigh the benefits by far, especially that even short to medium term use might bring measurable benefits, especially if accompanied by exercise and improved nutrition.
https://x.com/bryan_johnson/status/1885024727095529895#m
2 Likes
Can’t believe he even felt the tirzepatide at 500ug a week. I’m using 25 times his dosage
4 Likes
Davin8r
#38
He does make an interesting case for the negative health impact from the sleep disruption. My sleep was never perfect to begin with, but it’s certainly lower quality ever since I started down the GLP road.
1 Like
"A lower RHR is foundational to perfect sleep. The increase in my RHR decreased my HRV by 7 points and decreased sleep quality by 10%. "
When people say that something decreased their sleep quality by 10%, etc.
I say BS! You would have to do the results over an extended period of time while not changing any other variables.
Apparently at 84, I sleep better than Bryan Johnson.
If tirzepatide affected my sleep, I was unaware of it.
Maybe increasing his resting heart rate from 40 to 47 might be a healthy thing to do.
Is there any literature suggesting that a resting heart rate of 40 is healthy?
If my resting heart rate were 40, my doctor would probably refer me to a cardiologist.
I no longer care what Bryan Johnson is saying.
6 Likes
I would be curious what he means by reducing sleep quality by 10%. Historically he’s used the “sleep performance” score from whoop, which just measures that you’ve had sufficient sleep (ie duration). If he means sleep performance, it’s hard to see why RHR would impact that as it’s primarily a function of how long you spend in bed. Unless he’s suggesting that an increased RHR dramatically decreased his sleep efficiency by 10%, which I would respond by saying that seems highly unlikely.
1 Like
A_User
#41
If I’m going to speculate, it’s the same side effect that he prominently talked about as with rapamycin, coincidence? Hasn’t he detected any side effects from the few dozen pills (~100 interventions?), he does?
Optimizing certain biomarkers without knowing the causal pathway seems a bit low tier and not something you, to be honest, expect from someone who has a team and is dedicated to it as well. The mechanism of action matters as well. Otherwise it’s Goodhart’s law. It’s like optimizing grip strength because people who are frail and score low have increased mortality. So that doesn’t make you immortal because you keep increasing your strength because a bunch of people scored low & had increased mortality. Or they are using studies done on like 50 year olds, where a certain marker had a “decrease in all cause mortality”, but it’s about useless as it isn’t max lifespan, and the base rate is so low so the absolute risk is a rounding error. That’s the same thing with the VO2 Max study here: https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2707428 they did in in 53 year old with LOW BASE RATE mortality. It says little of maximum lifespan over a lifetime.
My point is I think you need to know HOW resting heart rate improves or increases mortality. Then you need to see if your intervention does it via that mechanism of action and actually see what the difference is on LIFETIME risk.
The sleep trackers like whoop isn’t totally accurate either. I’ve felt like I’ve had great sleep but the scores are low, it’s just dumb, it would be better with something that measures brainwaves.
I’m just a layman so I don’t know. Peter Attia loved that VO2 Max study.
2 Likes
cl-user
#42
He only finds side effects for prescription meds he can’t sell. 
6 Likes