@rivasp12
Re " Effect of sirolimus on carotid atherosclerosis in kidney transplant recipients: data derived from a prospective randomized controlled trial"
Although a positive (cIMT) small trial signal, I don’t think anywhere sufficient to answer this question definitively…certainly in the context of LIFELONG taking. Why didn’t they evaluate other CVD markers…VO2, CAC? They would not have been so onerous of tests at only 6 and 12 month intervals? They could have really done a better more fundamental physiological study.
An interesting observation from the study:
“In this study, cIMT was decreased in all patients (both groups) because of the transplant effect, which has already been observed in previous studies that compared cIMT before and after transplantation [19]. The reduction of cIMT may be one of the factors responsible for declining cardiovascular risk after kidney transplantation. In this study we also observed a class effect in which the sirolimus group had a greater reduction in cIMT; this was also seen in a model adjusted for principal factors associated with variability of cIMT”
But yet renal transplant patients have massively increased absolute CVD risk? So how to reconcile this short term cIMT improvement with very poor CVD outcome? We have some studies that show sirolimus + renal transplants have CVD lowering hazard ratios. So does this allow us to tease out a true sirolimus effect?
I found the comparative and changes in lipids very interesting (unusual?). Generally, positive or insignificant change, in both groups as well?
The paper references a cautionary note:
" Another point to consider in the pathophysiology of atherogenesis related to mTORI use is the time of exposure and the dose of these medications. The mTORI preferentially inhibit the
mTORC1 pathway, which is responsible for the major beneficial effects, including the anti-atherosclerotic responses. The inhibition of mTORC2, which was rapalog-insensitive, is related to increased insulin resistance and may be responsible for some serious undesired effects. Long-term treatment with mTORI may inhibit mTORC2 and may be responsible for the development of mTORC1 resistance, thus reversing its beneficial role in atherosclerosis [25]. This may explain the absence of effect on atherosclerosis in clinical trials with a long time of exposure to mTORI [15]"
Reference 15:
https://doi.org/10.1016/j.transproceed.2016.03.005
The study involved a group of 24 recipients treated with mTORi (mTORi group) and a group of 20 recipients treated with immunosuppressive regimen based on CNI (CNI group). [Carotid atherosclerosis was evaluated by measurement of the intima media thickness (IMT) of the common and internal carotid artery walls and detection of carotid plaques by a high-resolution
ultrasonography. The study was performed 3–24 years after transplantation. The mTORi group showed higher level of total cholesterol (242 vs 201 mg/dL), low-density lipoprotein cholesterol (140 vs 116 mg/dL), and triglycerides (226 vs 168 mg/dL). Post transplant diabetes developed in 34% of mTORi group compared with 25% in the CNI group. The mean of IMT (left and right) of common and internal carotid arteries was similar in both groups. Carotid plaques were detected in 46% of patients from the mTORi group and 25% from CNI group.The presence of carotid plaques combined with an IMT of >0.9 mm were associated with male gender, mTORi treatment and cardiovascular events. The incidence of coronary heart disease in mTORi group than in CNI group (53% vs 20%)
Conclusions
There was NO beneficial effect of immunosuppressive treatment with mTORi on carotid atherosclerosis in renal transplant patients.
What about larger, long term rapamycin HUMAN trials and CVD risk?
https://sci-hub.se/10.1034/j.1600-6143.2002.20610.x
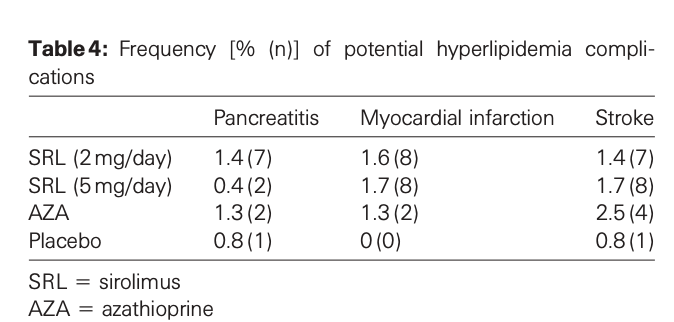
“Lipid data from two large controlled studies of 1295 renal transplant patients were analyzed retrospectively. Sirolimus 2mg/day and 5mg/day were compared with placebo or azathioprine, and administered concomitantly with steroids and cyclosporine over 12months. Hypercholesterolemia and hypertriglyceridemia occurred in all treatment groups and were maximal at 2–3months. The sirolimus groups evidenced higher lipid levels than the controls, but the elevations diminished over time. At 1 year, the patients given sirolimus 2mg/day had a mean cholesterol level 17mg/dL greater and a mean triglyceride level 59mg/dL greater than the controls. Among the patients given sirolimus 5mg/day, mean cholesterol was 30mg/dL greater and mean triglycerides were 103mg/dL greater than the controls. Treatment with statins and fibrates was effective in reducing cholesterol and triglyceride levels, respectively, in the sirolimus-treated patients. The Framingham risk model predicted that the 17mg/dL elevation in cholesterol would increase the incidence of coronary heart disease (CHD) by 1.5 new cases per 1000 persons per year and CHD death by 0.7 events per 1000 persons per year. Lipid elevations observed in the sirolimus-treated patients were manageable, improved over time, and responded to lipid-lowering therapy. Based on the Framingham risk model, the CHD risks associated with these cholesterol elevations are small compared with the baseline risks of the transplant population.”
“The impact of sirolimus on major coronary risk factors was limited to an increase in the total serum cholesterol level”
In this study, they used classic lipid lowering interventions to mediate CVD risk, including the Sirolimus group, so we don’t have a clear cut sirolimus ONLY intervention. 48% of sirolimus 2mg/day were put on a statin. But again, RENAL transplant cohort, not healthy persons.
I don’t think this question is settled. Is there a subset of rapamycin users where there is an actual anti-atherolosclerotic long term benefit? And what would be this phenotype? Excellent physical and metabolic health, with LOW baseline lipids and glucose, ABSENT CVD?? But wait, is this phenotype going to even have lifespan lowering via CVD as baseline risk? So what is sirolimus overlay doing? This phenotype might be able to dose at higher levels for OTHER all cause mortality reducing effects?
Or someone with good markers and some level of CVD (say low risk CAC)…is this phenotype going to benefit the most over long term? Can this phenotype ride out some level of dyslipidemia, and does it matter if not fully transient??